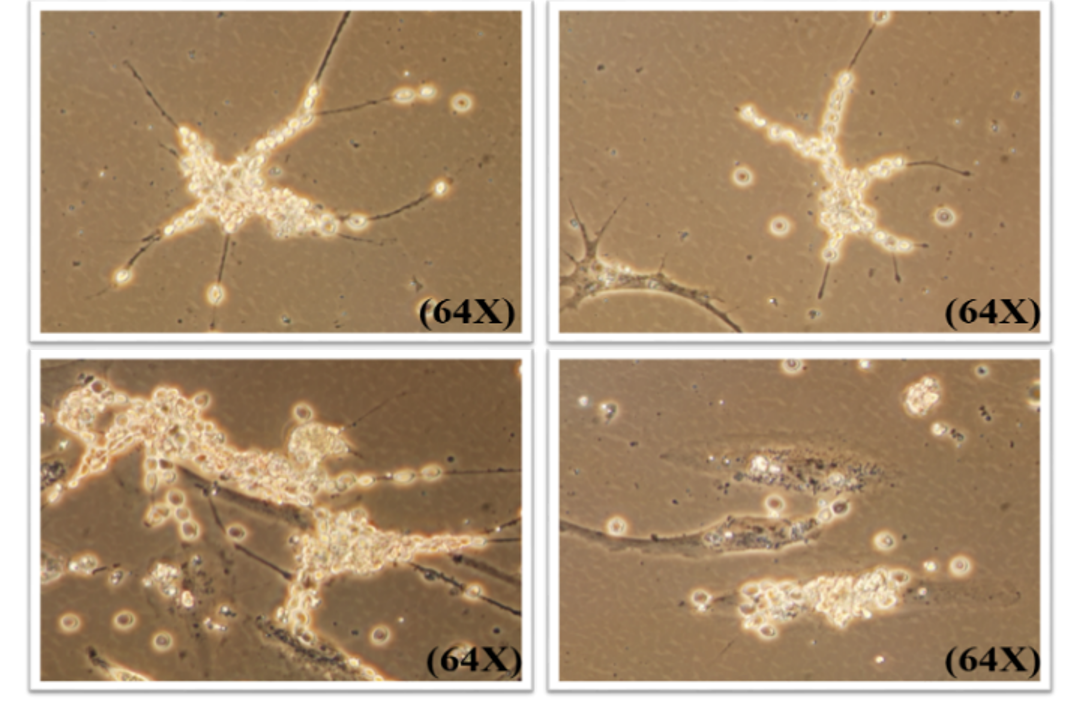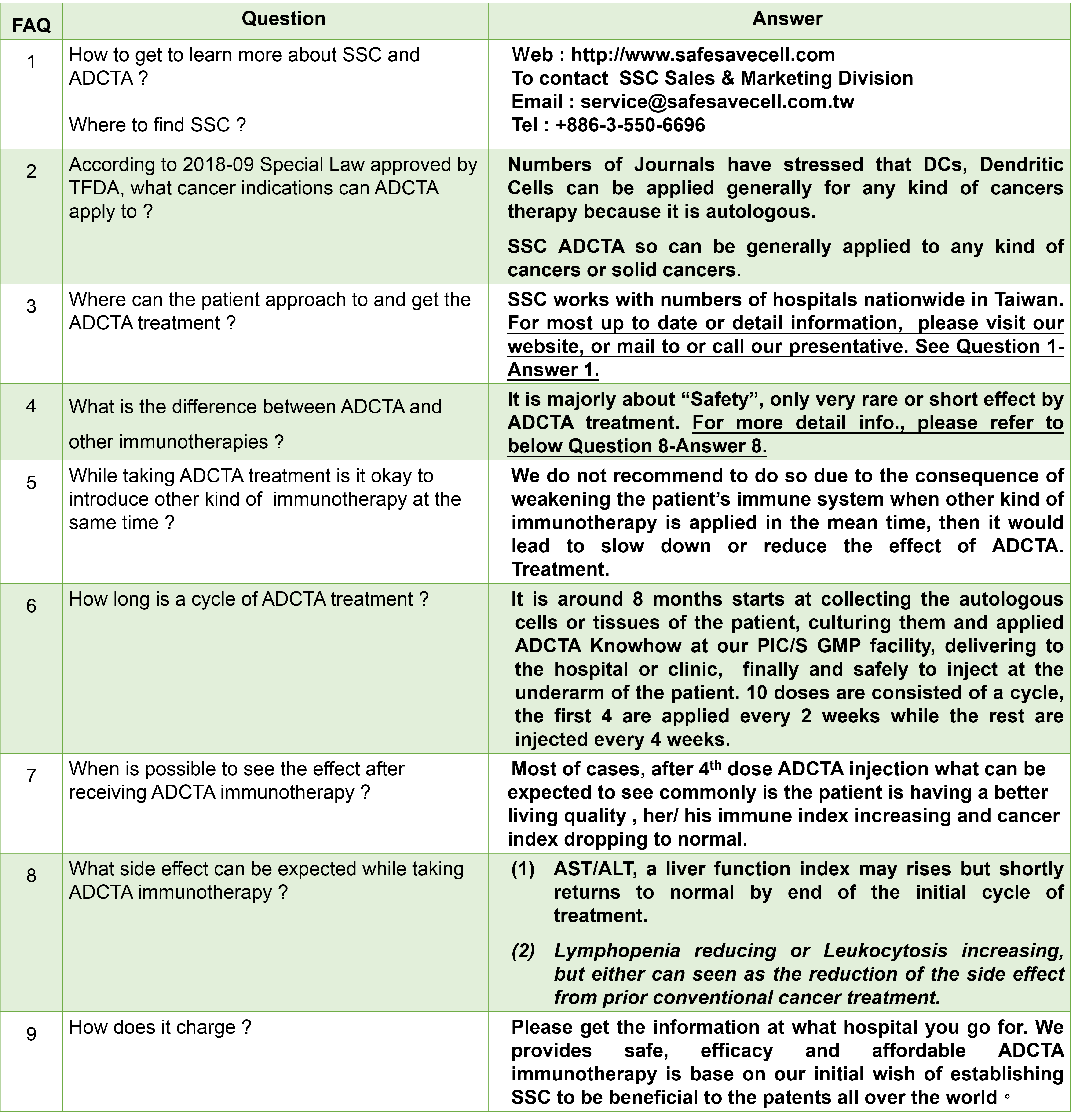


In early September 2018, the Ministry of Health and Welfare of Taiwan issued the revised provisions of the “Administrative Measures for the Implementation or Use of Medical Devices for Specific Medical Technology Inspection and Inspection”. The application of open cell therapy technology includes autoimmune cell therapy and cancer patients and entities for standard treatment failure. Patients with advanced cancer. The Shifu Cell Program will rapidly promote ADCTA to more drug-free or terminally fatal cancers, such as metastatic lung cancer, colorectal cancer, pancreatic cancer, prostate cancer, recurrent ovarian cancer, and breast cancer. Wait. Shifu Cell has cooperated with many hospitals in North, Central and South Taiwan, and has been able to formally serve Taiwan's medical technology and cancer patients in the near future. It has always adhered to the world's pioneering and therapeutic leader of Taiwan's immune cell therapy, and hopes to become a global standard for immune cell therapy through more successful cases of treating clinical patients.
Cell storage process

Several kinds of immunocyte in the human blood have their own responsibility, for example, red blood cells carry oxygen, platelets work to clot blood, blood plasmas transport nutrients, wastes and regulate physiological condition as well as white blood cells fight against diseases. Those immunocyte travel and can be seen all over the human body via our circulatory system, they are responsible for logistics and defense etc. to maintain a human life. There are 3 common types of Immunocyte as below:
Around 60% ~ 70% of white cell is neutrophil, it usually moves first to where is affected by bacterial or fungal infection due to chemotaxis. It often effects acute inflammation after phagocytosing small amount of pathogens. Stopping renew itself lysosomes causes die and becoming purulent.
Around 0.5% ~ 5% of white cell is eosinophil, it has less capability compared to neutrophil to phagocytose the pathogens. Its function is to regulate allergy and resist parasites.
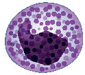
Less than 1% of white cell is eosinophil, it is similar to eosinophil doing resisting parasites, besides, it plays an important role in resisting inflammatory and allergy by not just consisting of the vasodilator “histamine” which increases blood flow to tissues but also the anticoagulant “heparin” which prevents blood from clotting blood quickly.
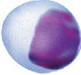
A type of lymphocytes, it is differentiated from thymus and becoming mature before transferring to lymphoid. By functions, 4 categories of Helper, Regulatory, Memory and Killer by different functions are majorly listed. It is kid of cell immunity of adaptive immunity

A type of lymphocytes, it becomes mature in the human bone. When antigen exists it starts to differentiate into plasma cells to release antibody. It is kind of humoral immunity of adaptive immunity.
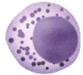
A type of lymphocytes, it is a non-specific congenital immunity, when a human is likely be getting infected by virus or cancer cell exists it can speedily release kinds of cytotoxin, such as perforin to lead those virus or cells to death.
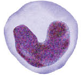
Around 3% ~ 8% of white cell is monocyte, it is the largest volume of white cells. It acts not just as neutrophil to phagocytose the pathogen but also is able to renew itself lysosome and after metabolized to bring the pathogen debris to T cells, which can specifically identify and kill the pathogen. Successfully bridging the innate and adaptive immunity allows mononuclear migrates from blood to tissues and differentiate into Macrophage or Dendritic Cells.
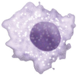
The most efficient phagocytosis cells, it stays in tissue and dis able to phagocytose the dead cells, cells decries or pathogens, their lysosome can simultaneously digest more than a hundred bacteria, after metabolized bring the pathogen debris to T cells and activate lymphocytes or other immune cells to help to speed up the response time to pathogens.
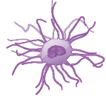
Originated in mononuclear, they are named because of its shape. well known for the most efficient antigen presenting ability. They can be seen at skin, lung, intestine, visualized inner of tissues or
Immature blood. After being activated it moves to lymph nodes to interact with T Cells and B Cells to initiate adaptive immunity.
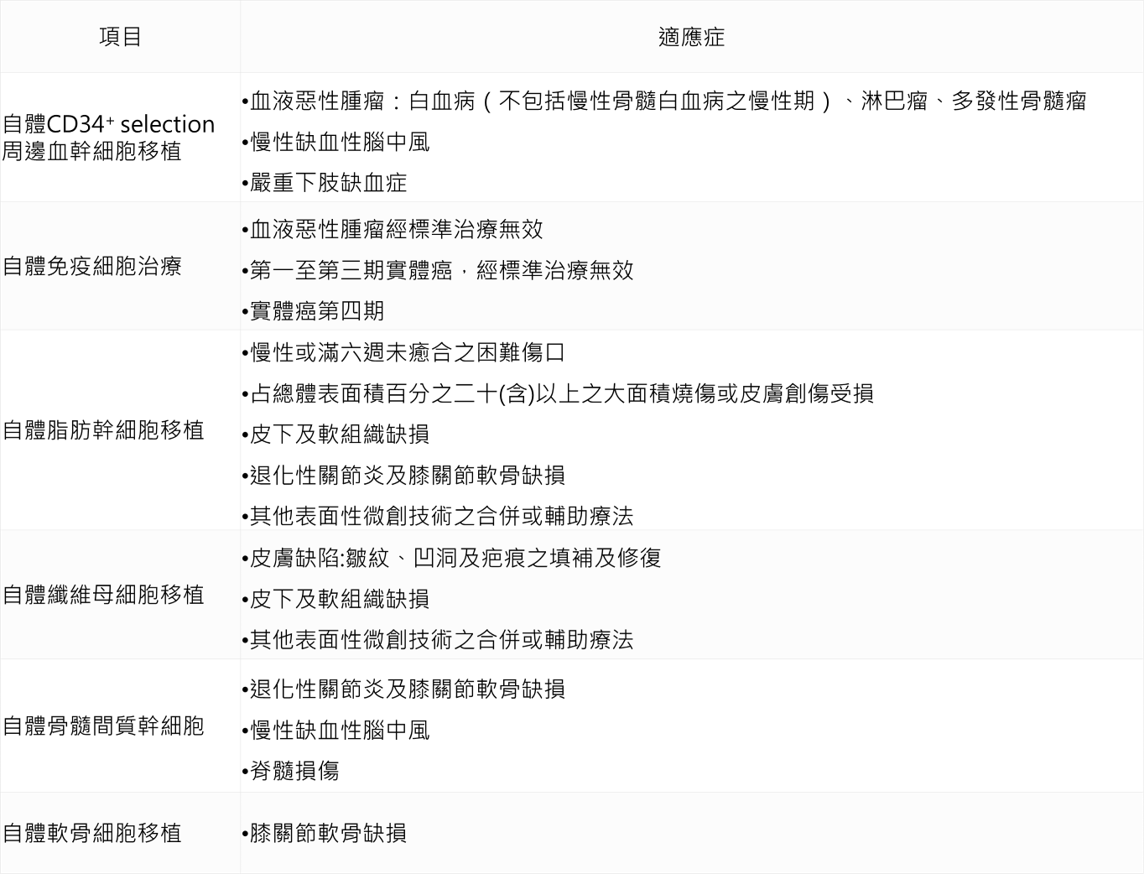
On September 4, 107, Weifu Department issued the “Administrative Measures for the Implementation or Use of Medical Devices for Specific Medical Technology Inspection and Inspection” (referred to as the special management method). On September 6, the six cell therapy technologies were officially opened, including the self-contained CD34+ selection. Blood stem cell transplantation, autoimmune cell therapy, autologous adipose stem cell transplantation, autologous fibroblast transplantation, autologous bone marrow mesenchymal stem cell transplantation, autologous chondrocyte transplantation.
Cancer Immunotherapy
The conventional cancer therapies have been poorly satisfied due to they have non-specificity, passiveness, limited efficacy and unbearable side effects. To the contrast, while the emerging immunotherapy focus on stimulating the immune system to awake the vital specific and active auto-immunocyte to be able to be targeting on attacking and destroying the remaining cancer cells after surgery to result a much better efficacy in longer life and living quality of a patient after receiving a radiotherapy or chemotherapy.
Immunotherapy emphases on strengthening the autoimmune system of a patient or obtaining the capability of immunity to prevent or cure patient’s disease. The advantage of introducing an immunotherapy is what Specificity, Efficiency and Lasting can be expected. This technology makes use of the human immune system and adopts a medical technic for the cancer patient. Among with 3 conventional treatments of surgery, radiotherapy and chemotherapy, the public worldwide has very high expectation ever since to consider the immunotherapy to be the 4th treatment on the list of options.

Passive Immunity
The way of Passive Immunity is to have patients receive allogeneic antibodies in order to inhibit the cancer cells metastasis or to kill the cancer cells.
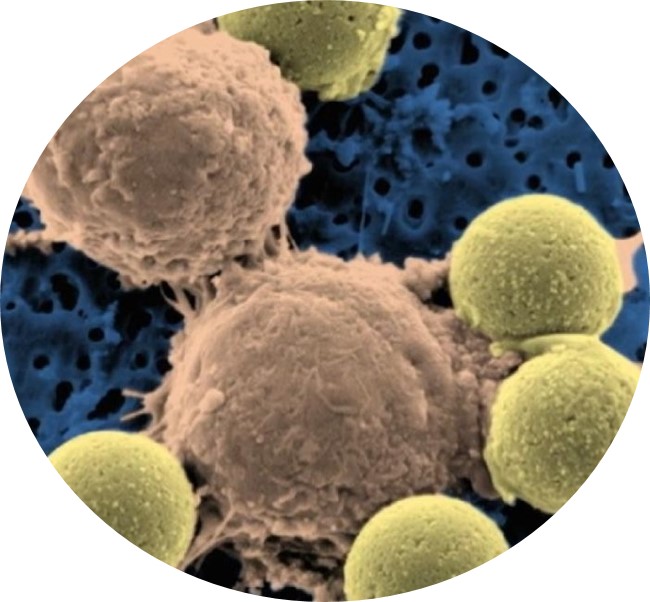
Active Immunity
The active immunity is also known as cancer vaccine, divided into 3 categories as Tumor Cell Vaccine, Tumor Antigen Vaccine and Cell Antigen. It uses human’s tumor debris, synthetic peptide drugs or applying the adoptive immunotherapy to increase the patients’ immunity.
Dendritic cell immunotherapy
Dendritic cells originate in human hematopoietic stem cells within bones marrow, the differentiation process begins with the stem cells differentiate into bone marrow precursor cells, then mononuclear and eventually dendritic cells.
Besides DC has the best antigen presenting ability it plays also a significant role in inducing congenital and acquired immune ability. Technologically when DC manipulates the tumor antigen under the most favorable conditions in vitro, DC then becomes a vaccine carrying tumor antigen and ready for injecting to the patient to re-simulates or re-activates cancer killer T cells ability to suppress the grow of cancer.